

Document Type : Case Report
Authors
1 Urology and Nephrology Research Center, Shahid Labbafinejad Hospital, Shahid Beheshti University of Medical Sciences, Tehran, Iran
2 Department of Surgery, Yas Hospital, Tehran University of Medical Sciences, Tehran, Iran
Abstract
Highlights
Keywords
Introduction
Mucinous cystadenoma may commonly arise from the ovary or pancreas however primary retroperitoneal mucinous cystadenoma (PRMC) is a rare cystic tumor and to our knowledge, less than 50 cases have been reported and published in the literature (1, 2). Due to the possible malignant potential of the lesion, complete resection of the cyst is highly recommended (3, 4). Herein we describe a 47-year-old woman with primary retroperitoneal mucinous cystadenoma. The presented case would be the second one reported in Iran (5). We explained clinical data, imaging studies, management, histopathology report, and follow-up of the lesion.
Case presentation
A 47-year-old woman presented with vague abdominal discomfort for six months. The informed consent was completed by the patient to report the case, and the case was reported based on CARE guidelines.
The patient and her family had always lived an urban life and they didn’t have any close contact with farm animals and their products. She didn’t mention any history of malignant or benign abdominal tumors in her first-degree relatives. In physical examination, a mobile palpable mass with mild tenderness located in the left flank region was noticed. Pelvic examination was normal. She had a history of umbilical hernia repair two years ago. Routine lab tests were all within normal limits. Tumor markers including carcinoembryonic antigen (CEA), cancer antigen 125 (CA 125), and carbohydrate antigen 19-9 (CA19-9), and blood biochemistry seemed to be normal. An ultrasound study showed a huge cystic lesion adjacent to the left kidney. Abdominopelvic computed tomography scan (CT scan) demonstrated a homogeneous unilocular cystic lesion in the retroperitoneal space measuring about 20x15 cm with no enhancement (Figure1a). The left kidney and descending colon were displaced medially by the mass (Figure1b). The aspect was compatible with a huge retroperitoneal cyst.
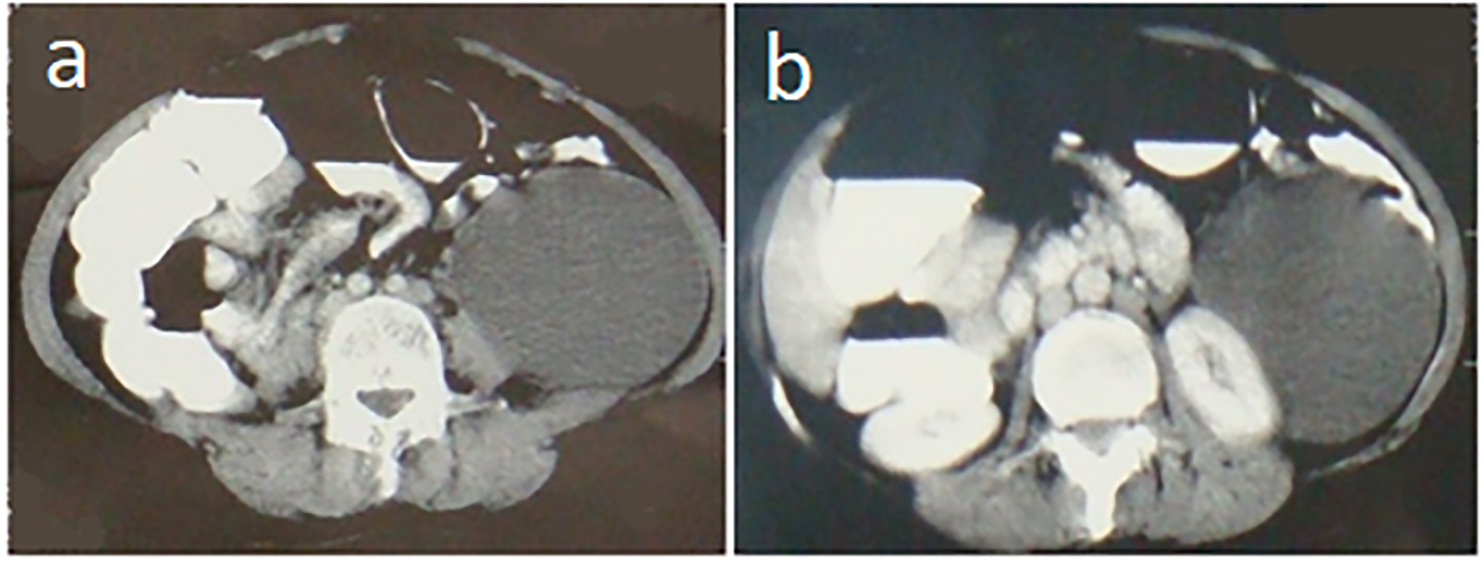
Figure 1. (a) Abdominopelvic CT scan demonstrated a homogeneous unilocular cystic lesion in the retroperitoneal space measuring about 20x15 cm with no enhancement, (b) with mild adhesions to the lower pole of the left kidney
The patient underwent exploratory laparotomy through a midline incision. A massive retroperitoneal cystic lesion was identified with mild adhesions to the lower pole of the left kidney and descending colon (Figure 2a, b). The mass was gently dissected from the adjacent organs and removed completely without spillage of its content. Pancreas, ovaries, uterus, fallopian tubes, and appendix seemed normal in size, appearance, and location.

Figure 2. (a, b) A 19x14x8 cm primary retroperitoneal cystadenoma with mild adhesions to descending colon. The cyst is shown in this image of two facades
The patient has discharged in 2 days and the post-operative course was uneventful. In the histopathology report, findings were compatible with a 19x14x8 cm unilocular benign primary retroperitoneal mucinous cystadenoma. In the histologic exam, the wall of the cyst was composed of thick fasciculated fibrous and hyalinized tissue covered by mucus-secreting cells (Figure 3a, b). In three years of follow-up of the patient with biannual ultrasound study and yearly CT scan, we didn't find any recurrence of the lesion.

Figure 3. (a, b) In a histologic exam, the wall of the cyst was composed of thick fasciculated fibrous and hyalinized tissue covered by mucus-secreting cells
Discussion
Mucinous cystadenoma arising from the ovary or pancreas is a relatively prevalent cystic lesion, however primary retroperitoneal mucinous cystadenoma is an extremely uncommon tumor (1, 6). Most of the lesions are asymptomatic and are discovered incidentally after a routine checkup evaluation. Signs and symptoms related to this lesion are mostly due to their large size and pressure effect on adjacent organs. This pathology usually occurs in women and most of them complain of vague abdominal discomfort. Its etiology is not clear. It may arise from ectopic ovarian, pancreatic, or appendicular tissue (1, 3, 4).
Indicating the exact location of the cyst in imaging studies would be very difficult and challenging especially in patients with a history of surgery (2, 3). Detecting a retroperitoneal cyst in ultrasound study mandates further radiologic evaluation (7). CT scan is the gold standard imaging modality for diagnosis and detecting some features of retroperitoneal cysts including location and size of the cyst, wall thickness, and presence of calcifications, enhancement pattern, cyst wall regularity, invasion of the adjacent organs, fat, myxoid stroma, and necrosis. Nevertheless, magnetic resonance imaging (MRI) in comparison with CT scan, can detect enhancing intra-lesion septae or nodules as well as more accurate localization and extension (8).
Differential diagnosis of PRMC includes lymphangioma, cystic mesothelioma, cystic teratoma, and non-pancreatic pseudocyst (7). Cystic lymphangioma usually contains septic, cystic mesothelioma contains a clear watery fluid, and patients with non-pancreatic pseudocyst have a history of inflammatory pancreatic disease. Cystic teratoma contains a fat component within a predominant liquid component (1, 2, 4).
Hydatid cyst is one of the differential diagnoses of retroperitoneal cysts and it would be better if we had performed serological laboratory tests to rule out this diagnosis. However, lacking any calcification, septation, or anything suspicious for existing daughter cysts in imaging studies, were the main reasons to proceed with the case with surgery.
Once the tumor is diagnosed, complete resection should be considered due to the malignant or infectious potential of the lesion (1, 3). An exploratory laparotomy with complete enucleation is the traditional treatment (9). Since our patient had a history of umbilical hernia repair, we decided to perform an open laparotomy exploration. Laparoscopic excision is safe and feasible if done by an expert laparoscopic surgeon (8). It is important to note that cystic fluid spillage has to be prevented due to the uncertain pathology of the tumor in most of cases (9).
A definitive diagnosis will be based on a histologic exam. PRMC is a cystic tumor lined by a single layer of uniform columnar cells with abundant intracytoplasmic mucin and small basal nuclei. Tumor markers such as CA 125, CA 19-9, alpha-fetoprotein (AFP), and CEA are in the normal range in these patients and wouldn’t help us in diagnosis and follow-up. These tumors are classified into mucinous cystadenomas, mucinous borderline tumors of low malignant potential, and mucinous cystadenocarcinoma. Retroperitoneal mucinous cystadenoma is the most common type and is usually presented as a large, unilocular, or multi-locular benign cystic. Tumor recurrence after resection is rare in this type. In the second type, the cells of the inner lining present with foci of epithelial proliferation. This type resembles the ovarian mucinous cystadenomas of low malignant potential. The third type is the mucinous cystadenocarcinoma that is an aggressive tumor in behavior (9).
Conclusions
Although primary retroperitoneal mucinous cystadenoma is a very rare entity, it should be considered in the differential diagnosis of any retroperitoneal cystic lesion. Since the definitive diagnosis of these lesions is made by histopathologic evaluation, complete resection of them is both diagnostic and therapeutic. Once the tumor is identified, immediate surgical removal is highly recommended due to their infectious or recurrence potential and possible malignant degeneration.
Authors’ Contribution
NM was responsible for study conception and design. MD provided data, and MP wrote the manuscript. MSH was responsible for supervision.
Acknowledgments
Special thanks to the Urology Research Center (URC), Tehran University of Medical Sciences (TUMS).
Conflict of interest
All authors claim that there is not any conflict of interest.
Funding
There is no funding.
Ethical Statement
All authors ensured our manuscript reporting adheres to CARE guidelines for reporting of case reports.
Data availability
Data will be provided by the corresponding author on request.
Abbreviation
AFP Alpha-fetoprotein
CA19-9 Carbohydrate antigen 19-9
CA 125 Cancer antigen 125
CEA Carcinoembryonic antigen
CT scan Computed tomography scan
MRI Magnetic resonance imaging
PRMC Primary retroperitoneal mucinous cystadenoma